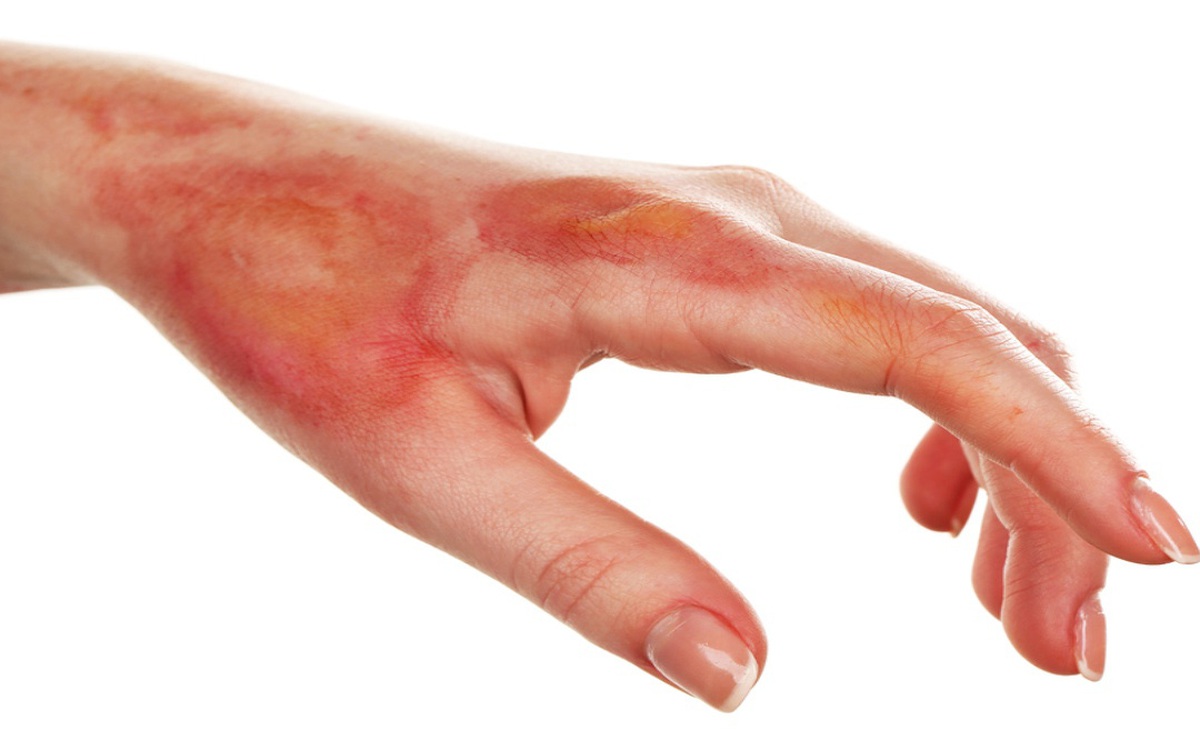
Burn injuries can have devastating physical and psychological consequences, often requiring long-term and intensive rehabilitation. These injuries can result from various causes, including accidents, fires, chemicals, and electrical incidents. Burn injury rehabilitation is a complex and multifaceted process that presents numerous challenges, but with the right approach and best practices, individuals can regain functionality and improve their quality of life.
Understanding Burn Injuries
Before delving into the rehabilitation process, it is essential to understand the different types of burn injuries and their severity. Burn injuries are categorized into three main degrees:
- First-degree burns: These are superficial burns that affect only the top layer of skin, causing redness and pain but generally healing on their own.
- Second-degree burns: These burns extend deeper into the skin and can cause blistering, swelling, and severe pain.
- Third-degree burns: The most severe type of burn, third-degree burns damage all layers of the skin and often extend into underlying tissues and organs. These injuries may appear charred, white, or black and can be painless due to nerve damage.
The extent of a burn injury is determined by the total body surface area (TBSA) affected and the depth of the burn. Rehabilitation requirements vary depending on these factors, with deeper and larger burns typically necessitating more extensive and prolonged rehabilitation.
Challenges in Burn Injury Rehabilitation
Rehabilitating burn injuries presents several unique challenges:
Pain Management:
Burn injuries are excruciatingly painful, and effective pain management is crucial throughout the rehabilitation process. Pain can hinder progress and negatively impact a patient’s mental and emotional well-being.
Scar Formation:
Scar tissue often forms as burn injuries heal, which can restrict joint movement and affect the appearance of the skin. Scar management is a vital component of rehabilitation, involving techniques such as pressure garments, silicone sheets, and scar massage.
Contractures and Functional Impairment:
Burn injuries can lead to contractures, where skin tightens and restricts joint movement. This can result in significant functional impairment, making it challenging for individuals to perform everyday tasks.
Psychological Impact:
The psychological impact of burn injuries is substantial. Patients may experience depression, anxiety, and post-traumatic stress disorder (PTSD). Addressing these mental health issues is essential for a successful rehabilitation process.
Nutritional Challenges:
Burn injuries often increase the body’s metabolic demands, requiring higher caloric intake and nutritional support to promote healing and tissue repair.
Infection Risk:
Burned skin is susceptible to infection, making infection prevention and control a top priority in burn units and during rehabilitation.
Long Duration:
Rehabilitation for severe burn injuries can be a lengthy process, sometimes taking years. Patients and their families must remain committed to the journey.
The best burn rehabilitation method
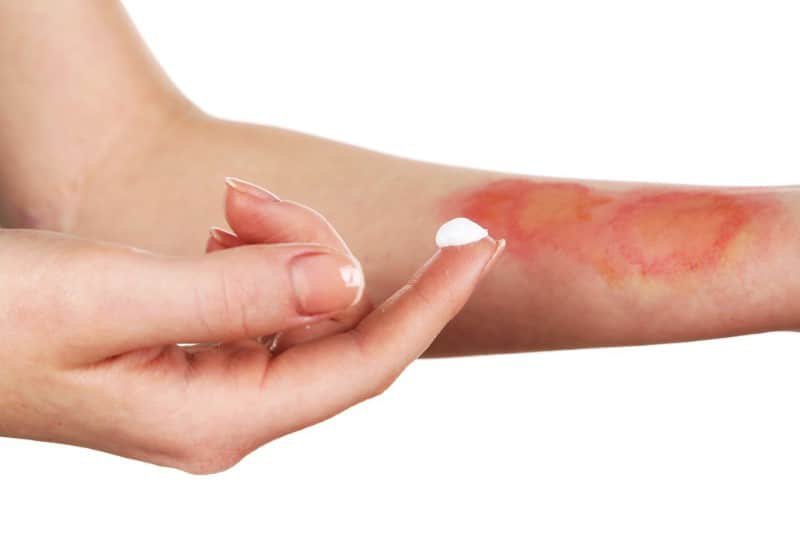
While the challenges in burn injury rehabilitation are significant, several best practices can help individuals on their road to recovery:
Multidisciplinary Approach:
A team of healthcare professionals, including burn surgeons, physical and occupational therapists, psychologists, and dietitians, should collaborate to address the physical, psychological, and emotional aspects of recovery.
Early Mobility:
Initiating mobility exercises as soon as possible helps prevent contractures and maintain joint flexibility. Physical therapists play a crucial role in this aspect.
Pain Management:
Effective pain management is paramount. This may involve medications, wound care techniques, and alternative therapies like relaxation techniques and distraction therapy.
Scar Management:
Starting scar management early can minimize the development of contractures and improve the appearance and functionality of the skin.
Psychological Support:
Psychological support, including therapy and counseling, should be readily available to address the emotional toll of burn injuries.
Nutritional Support:
Nutritionists and dietitians can develop personalized dietary plans to meet the increased energy and nutrient needs of burn patients.
Infection Control:
Strict infection control protocols, including wound care and hygiene practices, are essential to prevent complications.
Patient and Family Education:
Providing education to patients and their families about the rehabilitation process, home care, and support resources is crucial for long-term success.
Adaptive Equipment and Assistive Technology:
Assistive devices and technology can help individuals regain independence in daily activities.
Long-term Follow-up:
Burn injury rehabilitation is an ongoing process. Long-term follow-up care ensures that patients continue to progress and receive necessary support.
Conclusion
In conclusion, burn injury rehabilitation is a challenging but essential process that requires a comprehensive and multidisciplinary approach. Addressing pain, scar management, psychological well-being, and other aspects of recovery is crucial to help individuals regain their functionality and improve their overall quality of life. By implementing best practices and providing continuous support, healthcare professionals can make a significant difference in the lives of burn survivors.